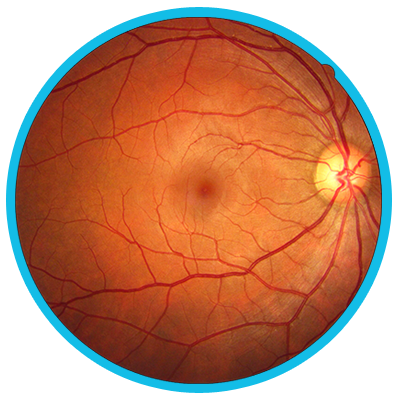
The most common mutation is in complement factor H ( CFH, chromosome 1q32-q32.1), but other complement pathway genes have been associated with the disease including CFI, MCP, CFB, and CFHR5. The major derangement in C3 glomerulopathy and the associated retinal disease is the alternative complement pathway. Retinal changes have an early onset with the average age of 41☒1 years in one series and as early as the teenage years in another. The mean age of onset for kidney disease is age 30☑9 for C3GN and 19☑8 for DDD. The female-to-male ratio for kidney disease is 1:1 and retinal disease is 2.7:1 to 1:1.5. The associated retinal disease has less consensus of terminology and is referred to as glomerulopathy-associated drusen, glomerulonephritis-associated drusen, early-onset drusen, or basal laminar drusen.Ĭ3 glomerulopathies are rare disorders. Both DDD and C3GN fall under complement-mediated disease, as compared to immune complex-mediated disease. With new understanding of the disease, the underlying kidney disease that included MPGN has been reclassified to C3 glomerulopathies with subgroups named dense deposit disease (DDD) and C3 glomerulonephritis (C3GN). Previously, the underlying kidney disease associated with drusen in the retina was called type II membranoproliferative glomerulonephritis (MPGN). The classification of glomerulopathy has recently undergone changes, and the literature is beginning to adopt new terminology.  
Glomerulopathy-associated drusen (formerly type II membranoproliferative glomerulonephritis-associated drusen) DISCUSSION Etiology/Epidemiology No ocular structural cause was identified and her drusen remained stable without complications. She also had a new diagnosis of antiphospholipid antibody syndrome. She returned to clinic two years later with new shadows and glare in the left eye greater than the right, which began after a recent transient ischemic attack. Due to her distance from the University of Iowa, the patient decided to follow locally and only return if she developed visual symptoms. Additionally, she was provided an Amsler grid to monitor for new visual symptoms. She focused her efforts on minimizing her risk factors, including control of blood pressure, weight, diet, and avoidance of smoking. After careful counseling of the limited data on the treatment and prognosis for drusen in patients without AMD, she decided to restart her AREDS vitamins. The patient remained visually asymptomatic, and she continued to monitor her kidney function regularly with her nephrologist. Sorsby macular dystrophy ( TIMP3 mutation).North Carolina macular dystrophy ( PRDM13 mutation).familial dominant drusen, Malattia Leventinese, Doyne honeycomb retinal dystrophy due to EFEMP-1/fibulin-3 mutation) Autosomal dominant radial drusen (a.k.a.Pattern macular dystrophy ( PRPH2 mutation, ABCA4 mutation).Glomerulopathy-associated drusen (including C3 glomerulopathies).Age-related macular degeneration ( related case | related tutorial).There are more hyperfluorescent drusen than seen on fundoscopic exam. A few drusen were near, but not completely abutting the optic nerve.įigure 3: Representative fluorescein angiography photos of both eyes. There was more clustering of drusen in the temporal macula. Maculae: There were multiple small to medium sized, round, yellow drusen, some confluent in the macula and nasal to the nerve in both eyes.Anterior chamber: Deep and quiet, both eyes.OS: 5 mm in dark, 3 mm in light, no RAPD.OD: 5 mm in dark, 3 mm in light, no relative afferent pupillary defect (RAPD).Otherwise negative except for what is detailed in the history of present illness. No other known affected family members, including her four children, and no known family history of renal disease. She did not know at what age her grandmother presented with signs of AMD. Past Ocular HistoryĮnd-stage renal disease, atopic rhinitis, degeneration of intervertebral lumbar disc, Hashimoto thyroiditis, obesity, anxiety, and depression Medicationsįamily history is notable for a maternal grandmother with AMD. The ophthalmologist described early-onset age-related macular degeneration (AMD) without visual changes, and the patient was referred to the University of Iowa.Īt her evaluation at the University of Iowa, she did not report any visual problems, including no decreased visual acuity, night blindness, metamorphopsia, scotomata, photophobia, pain, flashes, nor floaters. She was recommended to begin Age-Related Eye Disease Study (AREDS) formulation vitamins and told to follow up with an ophthalmologist at her next annual exam. The patient is a 32-year-old female who was noted to have macular changes in the absence of visual changes on a routine exam by an optometrist. "I don't have any problems with my vision, but my optometrist saw changes in my retina that I want a diagnosis for." History of Present Illness
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
